Condition Polymyalgia rheumatica. Polymyalgia rheumatica (PMR) This booklet provides information and answers to your questions about this condition.
|
|
|
- Ήράκλειτος Ζάχος
- 10 χρόνια πριν
- Προβολές:
Transcript
1 Condition Polymyalgia rheumatica Polymyalgia rheumatica (PMR) This booklet provides information and answers to your questions about this condition.
2 What is polymyalgia rheumatica? Polymyalgia rheumatica (PMR) is a condition that causes severe stiffness and pain, mainly in the muscles of the shoulders and thighs. In this booklet we ll explain the main symptoms of PMR and how it can be treated. We ll also suggest some sources of further information and support. At the back of this booklet you ll find a brief glossary of medical words - we ve underlined these when they re first used in the booklet.
3 Arthritis Research UK Polymyalgia rheumatica What s inside? 3 Polymyalgia rheumatica (PMR) at a glance 4 What is polymyalgia rheumatica (PMR)? 4 What are the symptoms of PMR? 4 Related condition: Giant cell arteritis 7 How is PMR diagnosed? 8 What treatments are there for PMR? Steroid tablets Other treatments 10 Self-help and daily living Exercise Diet and nutrition 12 Glossary 14 Where can I find out more? 16 We re here to help
4 2 Polymyalgia rheumatica (PMR) most commonly starts after the age of 60, though it can start as early as 50, and affects women more often than men.
5 At a glance Polymyalgia rheumatica (PMR) How is PMR diagnosed? PMR is usually diagnosed by your GP, based on your symptoms, the history of your condition and blood tests which will show inflammation. Your doctor may refer you to a specialist if the diagnosis isn t clear because several other conditions (including rheumatoid arthritis) may have similar symptoms in the early stages. Your doctor will want to check up on you regularly after treatment is started and do further tests to monitor your condition and treatment. What treatments are there? PMR is usually treated with steroid tablets. These often start to work very quickly but will need to be continued for some time to keep the inflammation under control and prevent the symptoms coming back. Your doctor will keep the dose of steroids as low as possible. How can I help myself? While you re taking steroids, it s important to make sure you get enough calcium and vitamin D, and your GP may prescribe treatment that will help to maintain bone strength. Weight-bearing exercise such as walking will also help to keep your bones strong and healthy. PMR is an inflammatory condition that causes very painful muscles. What related problems might occur? PMR is sometimes associated with inflammation of the arteries in the head, a condition called giant cell arteritis or temporal arteritis. This needs prompt medical treatment to protect your vision. You should see your doctor straight away if you have any of the following symptoms: severe headaches tenderness or swelling at the temples blurred or double vision jaw, tongue or facial pain especially when chewing. If your doctor suspects giant cell arteritis, you may be referred to a specialist and will be asked to have a biopsy of the temporal artery. However, your doctor may start you on a high dose of steroids even before you see the specialist as a precaution against possible loss of vision. 3
6 What is polymyalgia rheumatica (PMR)? Polymyalgia rheumatica (usually shortened to PMR) is an inflammatory condition that causes many (poly) painful muscles (myalgia). It tends to mainly affect the muscles of the shoulders and thighs. PMR can start at any age from 50 but mainly affects people over the age of 60. Women are affected 2 3 times as often as men and it affects about 1 in 2,000 people. What are the symptoms of PMR? If you have PMR you ll have severe and painful stiffness in the morning, especially in your shoulders and thighs. PMR often strikes suddenly, appearing over a week or two and sometimes just after a flu-like illness. The stiffness may be so severe that dressing, reaching, climbing stairs or even getting out of bed may be difficult. The symptoms are quite different from the ache you may feel after exercise that your body isn t used to. The pain and stiffness is often widespread and is made worse by movement, but it may also wake you at night. It s also common to feel unwell or to have a slight fever, and you may lose weight. At times, tiredness can be overwhelming. The condition can also make you feel low and become depressed. Related condition Giant cell arteritis PMR is sometimes associated with painful inflammation of the arteries of the skull. This is called giant cell arteritis (GCA) or temporal arteritis and needs prompt treatment as there s a risk of damage to the arteries of the eye. About 20% of PMR patients also develop GCA, while 40 60% of patients with GCA have symptoms of PMR. The symptoms of GCA are: severe headaches and pain in the muscles of the head tenderness at the temples pain in the jaw, tongue or side of the face when chewing pain or swelling in the scalp blurred or double vision. See Arthritis Research UK booklet Giant cell arteritis. 4
7 Arthritis Research UK Polymyalgia rheumatica Effective treatments for PMR are available, and in most cases they ll bring a complete recovery over time. 5
8 There s no specific test to diagnose PMR, so your doctor may try a number of different tests.
9 Arthritis Research UK Polymyalgia rheumatica How is PMR diagnosed? Normally PMR will be diagnosed and treated by your GP. However, you may be referred to a rheumatologist if there s any doubt about the diagnosis or if there are complicating factors for example, if the symptoms don t improve with steroid treatment or if you have sideeffects from it. There s no specific test to diagnose PMR. Your doctor will make the diagnosis based on the history of your illness, a physical examination and blood tests for inflammation. There are three tests that may be used: erythrocyte sedimentation rate (ESR) plasma viscosity (PV) C-reactive protein (CRP). The presence of inflammation alone won t confirm the diagnosis of PMR. Inflammation is a feature of many other conditions, including rheumatoid arthritis, so your doctor will need to do some tests to rule these out. You may need to have tests such as x-rays or ultrasound scans of the shoulders and hips. Anaemia (a lack of red blood cells) is quite common in PMR so your doctor may test for this, although anaemia can also be a symptom of other conditions. If your doctor suspects giant cell arteritis, they may suggest a temporal artery biopsy, when a small piece of the artery is taken from the scalp and examined under a microscope (See Figure 1). Figure 1 Profile of the head showing the temporal artery Photography used with kind permission of Elsevier. Elsevier Taken from Practical Rheumatology, third edition. Edited by Marc C Hochberg, Alan J Silman, Josef S Smolen, Michael E Weinblatt and Michael H Weisman. 7
10 What treatments are there for PMR? Steroid tablets Standard painkillers or anti-inflammatory drugs alone aren t enough to ease the symptoms. However, steroid (corticosteroid) treatment is usually very effective. The body makes several of its own steroids (including one called cortisol) in the adrenal glands, which sit on top of the kidneys, and they play an important part in keeping you healthy for example, by maintaining blood pressure and balancing salt and water levels in the body. When corticosteroid drugs are given in doses larger than the amount we already have in our bodies, they can have a powerful effect in reducing inflammation. Steroids won t cure PMR but the symptoms often improve significantly within a day or two once steroid treatment is started. However, treatment usually needs to continue for 2 years or more to stop symptoms returning. The steroid tablet most often prescribed is prednisolone. In most cases an initial dose of 15 mg of prednisolone a day makes the symptoms disappear completely. However, if you have giant cell arteritis you ll need higher doses than this to begin with in order to protect your vision. See Arthritis Research UK drug leaflet Steroid tablets.
11 Arthritis Research UK Polymyalgia rheumatica After a time your doctor will try to gradually reduce the dose of steroids to avoid potential side-effects such as osteoporosis. The reduction will be made in stages depending mainly on your symptoms but helped by repeat ESR or CRP test results. If symptoms return when the dose is reduced, your doctor may have to increase the dose for a short time and then, after several weeks, try to reduce it again. Raised ESR or CRP test results alone don t necessarily mean your steroid dose needs to be increased. You shouldn t stop taking your steroid tablets or alter the dose unless advised by your doctor, even if your symptoms have completely cleared up. This is because your body stops producing its own steroids while you re taking steroid tablets and needs a period of time to resume normal production of natural steroids before the drug is stopped. Even when you feel well, your doctor may wish to see you regularly so that you can be assessed for signs of a relapse or sideeffects from the drugs. Your doctor may want to check your general health and you may also be asked to have a bone density (DEXA) scan to assess the strength of your bones. We recommend you carry a steroid card that shows what dose of steroid you re on and how long you ve been taking them. If you need to see another doctor, for example while you re away from home, show them the card depending on what treatment you need, the steroid dose may need to be adjusted. See Arthritis Research UK booklet Meet the rheumatology team. Other treatments Steroid treatments can increase the risk of developing osteoporosis, making your bones more likely to fracture or break in a fall. Your doctor will therefore advise on drugs to help guard against osteoporosis, such as bisphosphonates, including risedronate or alendronate. If your symptoms are mild, you may be advised to take painkillers, also known as analgesics (e.g. paracetamol), or non-steroidal anti-inflammatory drugs (NSAIDs) to help ease the pain and stiffness, along with small doses of steroid tablets. Symptoms often improve significantly within a day or two of starting steroid treatment. 9
12 If your symptoms don t improve with steroids, or if it s difficult to reduce the dose of steroids over a period of time, your doctor may want to get a specialist opinion to confirm the diagnosis and treatment. The specialist may decide to prescribe methotrexate tablets alongside the steroid tablets for better disease control. Methotrexate works by reducing the activity of the immune system and therefore reduces inflammation. If you do need methotrexate it s important to have regular check-ups and blood tests to monitor the side-effects of the drug. Methotrexate can cause adverse effects such as feeling sick and mouth ulcers. More rarely it can cause more serious side-effects in the blood, liver or lungs. Most of these are picked up by the regular blood tests and get better if the drug is stopped. Methotrexate is usually only given to people who ve had repeated relapses. As the methotrexate takes effect it s usually possible to reduce the steroid dose. See Arthritis Research UK drug leaflets Drugs for osteoporosis; Methotrexate; Non-steroidal antiinflammatory drugs. Self-help and daily living Because steroid treatment can increase the risk of osteoporosis, it s important to think about the other risk factors associated with this condition. Smoking or drinking a lot of alcohol will both increase your risk of developing osteoporosis, while a diet that contains plenty of calcium and vitamin D, combined with some weight-bearing exercise, will help to reduce your overall risk. Sitting for any length of time may cause stiffness, making activities such as driving more difficult. Stop from time to time on a long journey to stretch your legs, arms and shoulders. Simple measures like a hot bath or shower can help to ease pain and stiffness, either first thing in the morning or after exercise. See Arthritis Research UK booklets Diet and arthritis; Osteoporosis. Exercise You ll need to find the right balance between rest and activity. Too much exercise is likely to make your symptoms worse, but activity usually helps to ease morning stiffness. Physiotherapy, including range of movement exercises for the shoulders, can be helpful in reducing pain and maintaining mobility. Weight-bearing exercise (any exercise that involves walking or running) is best for maintaining bone strength and guarding against osteoporosis, but walking is usually more suitable for people with PMR. 10
13 Arthritis Research UK Polymyalgia rheumatica Figure 2 Approximate calcium content of some common foods Food 115 g (4 oz) whitebait (fried in flour) 60 g (2 oz) sardines (including bones) 0.2 litre ( 1 3 pint) semiskimmed milk Calcium content 980 mg 260 mg 230 mg 0.2 litre ( 1 3 pint) whole milk 220 mg 3 large slices brown or 215 mg white bread 125 g (4 1 2 oz) low-fat yogurt 205 mg 30 g (1 oz) hard cheese 190 mg 0.2 litre ( 1 3 pint) calcium-enriched 180 mg soya milk 125 g (4 1 2 oz) calcium-enriched 150 mg soya yogurt 115 g (4 oz) cottage cheese 145 mg 3 large slices wholemeal bread 125 mg 115 g (4 oz) baked beans 60 mg 115 g (4 oz) boiled cabbage 40 mg Note: measures shown in ounces or pints are approximate conversions only. Diet and nutrition Steroid treatments reduce the amount of calcium absorbed from the gut and increase calcium loss through the kidneys. To counteract this we recommend a daily intake of calcium of 1,000 milligrams (mg) or 1,500 mg if you re over 60. A pint of milk a day, together with a reasonable amount of other foods that contain calcium, should be enough (see Figure 2). Vitamin D is sometimes called the sunshine vitamin because it s produced by the body when the skin is exposed to sunlight. It s also obtained from some foods, especially oily fish, and is added to some soya milks and vegetable margarines. It s sometimes necessary to take a daily supplement containing micrograms (μg) (this is the same as 400 to 800 international units (IU)) of vitamin D, especially for people over 60.
14 Glossary Anaemia a shortage of haemoglobin (oxygen-carrying pigment) in the blood which makes it more difficult for the blood to carry oxygen around the body. Anaemia can be caused by some rheumatic diseases such as rheumatoid arthritis or lupus, or by a shortage of iron in the diet. It can also be a side-effect of some drugs used to treat arthritis. Analgesics painkillers. As well as dulling pain they lower raised body temperature, and most of them reduce inflammation. Biopsy the removal of a small amount of living tissue from the body. The sample can help diagnose illness when examined under a microscope. Bisphosphonates drugs used to prevent the loss of bone mass and treat bone disorders such as osteoporosis. They work by reducing high levels of calcium in the blood and by slowing down bone metabolism. C-reactive protein (CRP) a protein found in the blood. The level of C-reactive protein in the blood rises in response to inflammation and a blood test for the protein can therefore be used as a measure of inflammation or disease activity. DEXA (dual-energy x-ray absorptiometry) a scan to test the strength or density of the bones. It involves lying on a couch, fully clothed, for about 15 minutes while your bones are x-rayed. The dose of x-rays is tiny about the same as spending a day out in the sun. The results will tell how much risk there is of the bones fracturing. 12 Erythrocyte sedimentation rate (ESR) a test that shows the level of inflammation in the body and can help in the diagnosis of a number of inflammatory conditions. Blood is separated in a machine with a rapidly rotating container (a centrifuge), then left to stand in a test tube. The ESR test measures the speed at which the red blood cells (erythrocytes) settle. Immune system the tissues that enable the body to resist infection. They include the thymus (the gland that lies behind the breastbone), the bone marrow and the lymph nodes. Inflammation a normal reaction to injury or infection of living tissues. The flow of blood increases, resulting in heat and redness in the affected tissues, and fluid and cells leak into the tissue, causing swelling. Non-steroidal anti-inflammatory drugs (NSAIDs) a large family of drugs prescribed for different kinds of arthritis that reduce inflammation and control pain, swelling and stiffness. Common examples include ibuprofen, naproxen and diclofenac. Osteoporosis a condition where bones become less dense and more fragile, which means they break, fracture or crumble more easily. Steroid treatment can increase the risk of developing osteoporosis. Plasma viscosity (PV) a screening test that measures the thickness or stickiness of the fluid in which blood cells are suspended. It s used as an indicator of disease activity in a number of conditions
15 Arthritis Research UK Polymyalgia rheumatica including rheumatoid arthritis, psoriatic arthritis and lupus. Rheumatoid arthritis an inflammatory disease affecting the joints, particularly the lining of the joint. It most commonly starts in the smaller joints in a symmetrical pattern that is, for example, in both hands or both wrists at once. Ultrasound scan a type of scan that uses high-frequency sound waves to examine and build up pictures of the inside of the body. 13
16 Where can I find out more? If you ve found this information useful you might be interested in these other titles from our range: Conditions Giant cell arteritis Osteoporosis Therapies Meet the rheumatology team Self-help and daily living Diet and arthritis Drug leaflets Drugs for osteoporosis Methotrexate Non-steroidal anti-inflammatory drugs Steroid tablets You can download all of our booklets and leaflets from our website or order them by contacting: Arthritis Research UK PO Box 177 Chesterfield, Derbyshire S41 7TQ Phone: Related organisations The following organisations may be able to provide additional advice and information: Arthritis Care 18 Stephenson Way London NW1 2HD Phone: Helpline: PMR GCA UK Centre for Disability Studies Adult Community College Rocheway, Rochford Essex SS4 1DQ Phone:
17 Arthritis Research UK Polymyalgia rheumatica Notes 15
18 Arthritis Research UK Copeman House, St Mary s Court, St Mary s Gate, Chesterfield, Derbyshire S41 7TD Tel calls charged at standard rate Registered Charity No Arthritis Research UK 2011 Published April /PMR/11-1
19 ΙΩΑΝΝΗΣ Γ. ΡΟΥΤΣΙΑΣ ΜΙΚΡΟΒΙΟΛΟΓΙΚΟ ΔΙΑΓΝΩΣΤΙΚΟ & ΕΡΕΥΝΗΤΙΚΟ ΕΡΓΑΣΤΗΡΙΟ ΜΙΚΡΟΒΙΟΛΟΓΙΚΟ ΔΙΑΓΝΩΣΤΙΚΟ ΙΑΤΡΕΙΟ
20 Το εργαστήριο µας αποτελεί ένα διαγνωστικό εργαστήριο αναφοράς, για την πραγµατοποίηση µικροβιολογικών, βιοχηµικών, αιµατολογικών, ανοσολογικών και ορµονολογικών εξετάσεων. Στο εργαστήριο µας επίσης εκτελού νται και πιο εξειδικευµένες εξετάσεις όπως µοριακός έλεγχος µε PCR (πχ( για την µέτρηση ιικού φορτίου, έλεγχο θροµβοφιλίας κλπ), ανοσολογικός έλεγχος δυσανεξίας σε διατροφικούς παράγοντες και µέτρηση Τ Τ λεµφοκυτταρικής ανοσολογικής απάντησης. Τέλος, εκτελούνται ερευνητικά πρωτόκολλα που περιλαµβάνουν ανά λυση βιολογικών δειγµάτων, στατιστική επεξεργασία α ποτελεσµάτων και ανάπτυξη ʺin ʺ houseʺ διαγνωστικών µεθόδων, όπως ELISA µε ʺcustom ʺ peptidesʺ κλπ Επιστηµονικός υπεύθυνος του εργαστηρίου είναι ο Δρ Ιωάννης Ρούτσιας. Είναι Χηµικός και Ιατρός Βιοπαθολό γος Μικροβιολόγος µε διδακτορικό δίπλωµα στην Ανο σολογία. Το ερευνητικό του έργο είναι σηµαντικό (συνολικό Impact Factor διεθνών δηµοσιεύσεων = 242) και διεθνώς αναγνωρισµένο (H index( = 18), έτυχε δε δέκατρι ων ελληνικών και διεθνών βραβείων και διακρίσεων. Αριστούχος υπότρο φος Χηµικός, εισήχθη και φοίτησε εν συνεχεία στην Ιατρική Σχολή του Πανεπιστηµίου Ιωαννίνων ( ) 1997) όπου και εκπόνησε και την διδακτορική του διατρι βή µε υποτροφία (ΕΜΥ). Έλαβε την ειδικότητα Μικροβιολογίας στην Αθήνα (Νοσ Παίδων Π&Α Κυριακού) και υπήρξε Λέκτορας ʺΙατρικής Ανοσοχηµείαςʺ στο Χ.Π.Α. ( ), 2004), ενώ από το 2004 έως το 2011 είναι Λέκτορας Ανοσολογίας/Μικροβιολογίας στην Ιατρι κή σχολή του Πανεπιστηµίου Αθηνών. Είναι συντάκτης κριτής σε 12 διεθνή περιοδικά, έχει δηµοσιεύσει 50 άρθρα σε διεθνή περιοδικά (µεσος IF/αρθρο=4.8) µε > 900 βιβλιο γραφικές αναφορές (cita ons).( Έχει επιβλέψει 12 διατριβές, έχει διδάξει 10 διαφορετικά αντικείµενα (µαθήµατα) σε 6 τµήµατα (Ιατρική, Οδοντιατρική, Φαρµακευτική, τµήµα Διαιτολογίας, Χηµικό, ΠΣΕ Βιοχηµείας) και έχει 146 ανα κοινώσεις σε συνέδρια (Ελληνικά: 53, Διεθνή: 93). Τέλος έχει γράψει κεφάλαια σε 6 διεθνή και 7 ελληνικά βιβλία και είναι µέλος σε 6 επιστηµονικές εταιρίες και συλλό γους. ΠΑΡΑΛΑΒΗ ΑΠΟΤΕΛΕΣΜΑΤΩΝ Αποτελέσµατα εξετάσεων: Οι ιατροί έχουν την δυνατό τητα να βλέπουν τα αποτελέσµατα των δικών τους ασθενών, ανά πάσα στιγµή, από την ιστοσελίδα του ιατρείου.
21 Μικροβιολογικό Διαγνωστικό Ιατρείο Υπεύθυνος: Ιωάννης Γ. Ρούτσιας, Λέκτορας Ιατρικής Σχολής Εθνικού και Καποδιστριακού Πανεπιστηµίου Αθηνών Διεύθυνση: Δ. Σούτσου 48 & Αλεξάνδρας Αµπελόκηποι, Αθήνα έναντι του σταθµού Μετρό (στάση Αµπελόκηποι) Τηλ: Fax: E mail: jroutsias@med.uoa.gr Web: lab.gr
Giant cell arteritis (temporal arteritis)
 Condition (temporal arteritis) This booklet provides information and answers to your questions about this condition. What is giant cell arteritis? (GCA) or temporal arteritis is an inflammatory condition
Condition (temporal arteritis) This booklet provides information and answers to your questions about this condition. What is giant cell arteritis? (GCA) or temporal arteritis is an inflammatory condition
Διαβητική αμφιβληστροειδοπάθεια
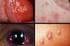
 Διαβητική αμφιβληστροειδοπάθεια Diabetic retinopathy Η εικόνα αυτή δείχνει ένα παράδειγμα του πώς μπορεί η διαβητική αμφιβληστροειδοπάθεια να επηρεάσει την όραση. Τι είναι η διαβητική αμφιβληστροειδοπάθεια;
Διαβητική αμφιβληστροειδοπάθεια Diabetic retinopathy Η εικόνα αυτή δείχνει ένα παράδειγμα του πώς μπορεί η διαβητική αμφιβληστροειδοπάθεια να επηρεάσει την όραση. Τι είναι η διαβητική αμφιβληστροειδοπάθεια;
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΤΜΗΜΑ ΝΟΣΗΛΕΥΤΙΚΗΣ
 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΤΜΗΜΑ ΝΟΣΗΛΕΥΤΙΚΗΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΨΥΧΟΛΟΓΙΚΕΣ ΕΠΙΠΤΩΣΕΙΣ ΣΕ ΓΥΝΑΙΚΕΣ ΜΕΤΑ ΑΠΟ ΜΑΣΤΕΚΤΟΜΗ ΓΕΩΡΓΙΑ ΤΡΙΣΟΚΚΑ Λευκωσία 2012 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΤΜΗΜΑ ΝΟΣΗΛΕΥΤΙΚΗΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΨΥΧΟΛΟΓΙΚΕΣ ΕΠΙΠΤΩΣΕΙΣ ΣΕ ΓΥΝΑΙΚΕΣ ΜΕΤΑ ΑΠΟ ΜΑΣΤΕΚΤΟΜΗ ΓΕΩΡΓΙΑ ΤΡΙΣΟΚΚΑ Λευκωσία 2012 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ
Osteoporosis. Condition. Osteoporosis. information and answers. to your questions about this condition. and answers to your questions
 Condition Osteoporosis Osteoporosis This This booklet leaflet provides provides information and answers to your questions information and answers about this condition. to your questions about this condition.
Condition Osteoporosis Osteoporosis This This booklet leaflet provides provides information and answers to your questions information and answers about this condition. to your questions about this condition.
Drugs and arthritis. Drug information Drugs and arthritis
 Drug information Drugs and arthritis Drugs and arthritis This leaflet provides information on drugs and arthritis and will answer any questions you have about the treatment. Arthritis Research UK produce
Drug information Drugs and arthritis Drugs and arthritis This leaflet provides information on drugs and arthritis and will answer any questions you have about the treatment. Arthritis Research UK produce
«ΨΥΧΙΚΗ ΥΓΕΙΑ ΚΑΙ ΣΕΞΟΥΑΛΙΚΗ» ΠΑΝΕΥΡΩΠΑΪΚΗ ΕΡΕΥΝΑ ΤΗΣ GAMIAN- EUROPE
 «ΨΥΧΙΚΗ ΥΓΕΙΑ ΚΑΙ ΣΕΞΟΥΑΛΙΚΗ» ΠΑΝΕΥΡΩΠΑΪΚΗ ΕΡΕΥΝΑ ΤΗΣ GAMIAN- EUROPE We would like to invite you to participate in GAMIAN- Europe research project. You should only participate if you want to and choosing
«ΨΥΧΙΚΗ ΥΓΕΙΑ ΚΑΙ ΣΕΞΟΥΑΛΙΚΗ» ΠΑΝΕΥΡΩΠΑΪΚΗ ΕΡΕΥΝΑ ΤΗΣ GAMIAN- EUROPE We would like to invite you to participate in GAMIAN- Europe research project. You should only participate if you want to and choosing
Instruction Execution Times
 1 C Execution Times InThisAppendix... Introduction DL330 Execution Times DL330P Execution Times DL340 Execution Times C-2 Execution Times Introduction Data Registers This appendix contains several tables
1 C Execution Times InThisAppendix... Introduction DL330 Execution Times DL330P Execution Times DL340 Execution Times C-2 Execution Times Introduction Data Registers This appendix contains several tables
Πώς μπορεί κανείς να έχει έναν διερμηνέα κατά την επίσκεψή του στον Οικογενειακό του Γιατρό στο Ίσλινγκτον Getting an interpreter when you visit your
 Πώς μπορεί κανείς να έχει έναν διερμηνέα κατά την επίσκεψή του στον Οικογενειακό του Γιατρό στο Ίσλινγκτον Getting an interpreter when you visit your GP practice in Islington Σε όλα τα Ιατρεία Οικογενειακού
Πώς μπορεί κανείς να έχει έναν διερμηνέα κατά την επίσκεψή του στον Οικογενειακό του Γιατρό στο Ίσλινγκτον Getting an interpreter when you visit your GP practice in Islington Σε όλα τα Ιατρεία Οικογενειακού
HOMEWORK 4 = G. In order to plot the stress versus the stretch we define a normalized stretch:
 HOMEWORK 4 Problem a For the fast loading case, we want to derive the relationship between P zz and λ z. We know that the nominal stress is expressed as: P zz = ψ λ z where λ z = λ λ z. Therefore, applying
HOMEWORK 4 Problem a For the fast loading case, we want to derive the relationship between P zz and λ z. We know that the nominal stress is expressed as: P zz = ψ λ z where λ z = λ λ z. Therefore, applying
(1) Describe the process by which mercury atoms become excited in a fluorescent tube (3)
 Q1. (a) A fluorescent tube is filled with mercury vapour at low pressure. In order to emit electromagnetic radiation the mercury atoms must first be excited. (i) What is meant by an excited atom? (1) (ii)
Q1. (a) A fluorescent tube is filled with mercury vapour at low pressure. In order to emit electromagnetic radiation the mercury atoms must first be excited. (i) What is meant by an excited atom? (1) (ii)
derivation of the Laplacian from rectangular to spherical coordinates
 derivation of the Laplacian from rectangular to spherical coordinates swapnizzle 03-03- :5:43 We begin by recognizing the familiar conversion from rectangular to spherical coordinates (note that φ is used
derivation of the Laplacian from rectangular to spherical coordinates swapnizzle 03-03- :5:43 We begin by recognizing the familiar conversion from rectangular to spherical coordinates (note that φ is used
Code Breaker. TEACHER s NOTES
 TEACHER s NOTES Time: 50 minutes Learning Outcomes: To relate the genetic code to the assembly of proteins To summarize factors that lead to different types of mutations To distinguish among positive,
TEACHER s NOTES Time: 50 minutes Learning Outcomes: To relate the genetic code to the assembly of proteins To summarize factors that lead to different types of mutations To distinguish among positive,
Phys460.nb Solution for the t-dependent Schrodinger s equation How did we find the solution? (not required)
 Phys460.nb 81 ψ n (t) is still the (same) eigenstate of H But for tdependent H. The answer is NO. 5.5.5. Solution for the tdependent Schrodinger s equation If we assume that at time t 0, the electron starts
Phys460.nb 81 ψ n (t) is still the (same) eigenstate of H But for tdependent H. The answer is NO. 5.5.5. Solution for the tdependent Schrodinger s equation If we assume that at time t 0, the electron starts
LESSON 6 (ΜΑΘΗΜΑ ΕΞΙ) REF : 201/045/26-ADV. 10 December 2013
 LESSON 6 (ΜΑΘΗΜΑ ΕΞΙ) REF : 201/045/26-ADV 10 December 2013 I get up/i stand up I wash myself I shave myself I comb myself I dress myself Once (one time) Twice (two times) Three times Salary/wage/pay Alone/only
LESSON 6 (ΜΑΘΗΜΑ ΕΞΙ) REF : 201/045/26-ADV 10 December 2013 I get up/i stand up I wash myself I shave myself I comb myself I dress myself Once (one time) Twice (two times) Three times Salary/wage/pay Alone/only
The Simply Typed Lambda Calculus
 Type Inference Instead of writing type annotations, can we use an algorithm to infer what the type annotations should be? That depends on the type system. For simple type systems the answer is yes, and
Type Inference Instead of writing type annotations, can we use an algorithm to infer what the type annotations should be? That depends on the type system. For simple type systems the answer is yes, and
Newborn Upfront Payment & Newborn Supplement
 GREEK Newborn Upfront Payment & Newborn Supplement Female 1: Το μωρό μου θα ρθει σύντομα, θα πρέπει να κανονίσω τα οικονομικά μου. Άκουσα ότι η κυβέρνηση δεν δίνει πλέον το Baby Bonus. Ξέρεις τίποτα γι
GREEK Newborn Upfront Payment & Newborn Supplement Female 1: Το μωρό μου θα ρθει σύντομα, θα πρέπει να κανονίσω τα οικονομικά μου. Άκουσα ότι η κυβέρνηση δεν δίνει πλέον το Baby Bonus. Ξέρεις τίποτα γι
ΑΓΓΛΙΚΗ ΓΛΩΣΣΑ ΣΕ ΕΙΔΙΚΑ ΘΕΜΑΤΑ ΔΙΕΘΝΩΝ ΣΧΕΣΕΩΝ & ΟΙΚΟΝΟΜΙΑΣ
 ΑΓΓΛΙΚΗ ΓΛΩΣΣΑ ΣΕ ΕΙΔΙΚΑ ΘΕΜΑΤΑ ΔΙΕΘΝΩΝ ΣΧΕΣΕΩΝ & ΟΙΚΟΝΟΜΙΑΣ Ενότητα 1β: Principles of PS Ιφιγένεια Μαχίλη Τμήμα Οικονομικών Επιστημών Άδειες Χρήσης Το παρόν εκπαιδευτικό υλικό υπόκειται σε άδειες χρήσης
ΑΓΓΛΙΚΗ ΓΛΩΣΣΑ ΣΕ ΕΙΔΙΚΑ ΘΕΜΑΤΑ ΔΙΕΘΝΩΝ ΣΧΕΣΕΩΝ & ΟΙΚΟΝΟΜΙΑΣ Ενότητα 1β: Principles of PS Ιφιγένεια Μαχίλη Τμήμα Οικονομικών Επιστημών Άδειες Χρήσης Το παρόν εκπαιδευτικό υλικό υπόκειται σε άδειες χρήσης
ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΠΛΗΡΟΦΟΡΙΚΗΣ CYPRUS COMPUTER SOCIETY ΠΑΓΚΥΠΡΙΟΣ ΜΑΘΗΤΙΚΟΣ ΔΙΑΓΩΝΙΣΜΟΣ ΠΛΗΡΟΦΟΡΙΚΗΣ 19/5/2007
 Οδηγίες: Να απαντηθούν όλες οι ερωτήσεις. Αν κάπου κάνετε κάποιες υποθέσεις να αναφερθούν στη σχετική ερώτηση. Όλα τα αρχεία που αναφέρονται στα προβλήματα βρίσκονται στον ίδιο φάκελο με το εκτελέσιμο
Οδηγίες: Να απαντηθούν όλες οι ερωτήσεις. Αν κάπου κάνετε κάποιες υποθέσεις να αναφερθούν στη σχετική ερώτηση. Όλα τα αρχεία που αναφέρονται στα προβλήματα βρίσκονται στον ίδιο φάκελο με το εκτελέσιμο
Other Test Constructions: Likelihood Ratio & Bayes Tests
 Other Test Constructions: Likelihood Ratio & Bayes Tests Side-Note: So far we have seen a few approaches for creating tests such as Neyman-Pearson Lemma ( most powerful tests of H 0 : θ = θ 0 vs H 1 :
Other Test Constructions: Likelihood Ratio & Bayes Tests Side-Note: So far we have seen a few approaches for creating tests such as Neyman-Pearson Lemma ( most powerful tests of H 0 : θ = θ 0 vs H 1 :
Paget s disease of bone
 Condition Paget s disease of bone Paget s disease of bone This booklet provides information and answers to your questions about this condition. What is Paget s disease of bone? Paget s disease of bone
Condition Paget s disease of bone Paget s disease of bone This booklet provides information and answers to your questions about this condition. What is Paget s disease of bone? Paget s disease of bone
Econ 2110: Fall 2008 Suggested Solutions to Problem Set 8 questions or comments to Dan Fetter 1
 Eon : Fall 8 Suggested Solutions to Problem Set 8 Email questions or omments to Dan Fetter Problem. Let X be a salar with density f(x, θ) (θx + θ) [ x ] with θ. (a) Find the most powerful level α test
Eon : Fall 8 Suggested Solutions to Problem Set 8 Email questions or omments to Dan Fetter Problem. Let X be a salar with density f(x, θ) (θx + θ) [ x ] with θ. (a) Find the most powerful level α test
HISTOGRAMS AND PERCENTILES What is the 25 th percentile of a histogram? What is the 50 th percentile for the cigarette histogram?
 HISTOGRAMS AND PERCENTILES What is the 25 th percentile of a histogram? The point on the horizontal axis such that of the area under the histogram lies to the left of that point (and to the right) What
HISTOGRAMS AND PERCENTILES What is the 25 th percentile of a histogram? The point on the horizontal axis such that of the area under the histogram lies to the left of that point (and to the right) What
EE512: Error Control Coding
 EE512: Error Control Coding Solution for Assignment on Finite Fields February 16, 2007 1. (a) Addition and Multiplication tables for GF (5) and GF (7) are shown in Tables 1 and 2. + 0 1 2 3 4 0 0 1 2 3
EE512: Error Control Coding Solution for Assignment on Finite Fields February 16, 2007 1. (a) Addition and Multiplication tables for GF (5) and GF (7) are shown in Tables 1 and 2. + 0 1 2 3 4 0 0 1 2 3
2 Composition. Invertible Mappings
 Arkansas Tech University MATH 4033: Elementary Modern Algebra Dr. Marcel B. Finan Composition. Invertible Mappings In this section we discuss two procedures for creating new mappings from old ones, namely,
Arkansas Tech University MATH 4033: Elementary Modern Algebra Dr. Marcel B. Finan Composition. Invertible Mappings In this section we discuss two procedures for creating new mappings from old ones, namely,
Στεγαστική δήλωση: Σχετικά με τις στεγαστικές υπηρεσίες που λαμβάνετε (Residential statement: About the residential services you get)
 Νόμος περί Αναπηριών 2006 (Disability Act 2006) Στεγαστική δήλωση: Σχετικά με τις στεγαστικές υπηρεσίες που λαμβάνετε (Residential statement: About the residential services you get) Greek Νόμος περί Αναπηριών
Νόμος περί Αναπηριών 2006 (Disability Act 2006) Στεγαστική δήλωση: Σχετικά με τις στεγαστικές υπηρεσίες που λαμβάνετε (Residential statement: About the residential services you get) Greek Νόμος περί Αναπηριών
MSM Men who have Sex with Men HIV -
 ,**, The Japanese Society for AIDS Research The Journal of AIDS Research HIV,0 + + + + +,,, +, : HIV : +322,*** HIV,0,, :., n,0,,. + 2 2, CD. +3-ml n,, AIDS 3 ARC 3 +* 1. A, MSM Men who have Sex with Men
,**, The Japanese Society for AIDS Research The Journal of AIDS Research HIV,0 + + + + +,,, +, : HIV : +322,*** HIV,0,, :., n,0,,. + 2 2, CD. +3-ml n,, AIDS 3 ARC 3 +* 1. A, MSM Men who have Sex with Men
9.09. # 1. Area inside the oval limaçon r = cos θ. To graph, start with θ = 0 so r = 6. Compute dr
 9.9 #. Area inside the oval limaçon r = + cos. To graph, start with = so r =. Compute d = sin. Interesting points are where d vanishes, or at =,,, etc. For these values of we compute r:,,, and the values
9.9 #. Area inside the oval limaçon r = + cos. To graph, start with = so r =. Compute d = sin. Interesting points are where d vanishes, or at =,,, etc. For these values of we compute r:,,, and the values
Right Rear Door. Let's now finish the door hinge saga with the right rear door
 Right Rear Door Let's now finish the door hinge saga with the right rear door You may have been already guessed my steps, so there is not much to describe in detail. Old upper one file:///c /Documents
Right Rear Door Let's now finish the door hinge saga with the right rear door You may have been already guessed my steps, so there is not much to describe in detail. Old upper one file:///c /Documents
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ. Πτυχιακή εργασία Η ΚΑΤΑΘΛΙΨΗ ΣΕ ΕΦΗΒΟΥΣ ΜΕ ΣΑΚΧΑΡΩΔΗ ΔΙΑΒΗΤΗ ΤΥΠΟΥ 1
 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ Πτυχιακή εργασία Η ΚΑΤΑΘΛΙΨΗ ΣΕ ΕΦΗΒΟΥΣ ΜΕ ΣΑΚΧΑΡΩΔΗ ΔΙΑΒΗΤΗ ΤΥΠΟΥ 1 ΑΝΔΡΕΑΣ ΑΝΔΡΕΟΥ Φ.Τ:2008670839 Λεμεσός 2014 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ Πτυχιακή εργασία Η ΚΑΤΑΘΛΙΨΗ ΣΕ ΕΦΗΒΟΥΣ ΜΕ ΣΑΚΧΑΡΩΔΗ ΔΙΑΒΗΤΗ ΤΥΠΟΥ 1 ΑΝΔΡΕΑΣ ΑΝΔΡΕΟΥ Φ.Τ:2008670839 Λεμεσός 2014 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ
Section 8.3 Trigonometric Equations
 99 Section 8. Trigonometric Equations Objective 1: Solve Equations Involving One Trigonometric Function. In this section and the next, we will exple how to solving equations involving trigonometric functions.
99 Section 8. Trigonometric Equations Objective 1: Solve Equations Involving One Trigonometric Function. In this section and the next, we will exple how to solving equations involving trigonometric functions.
C.S. 430 Assignment 6, Sample Solutions
 C.S. 430 Assignment 6, Sample Solutions Paul Liu November 15, 2007 Note that these are sample solutions only; in many cases there were many acceptable answers. 1 Reynolds Problem 10.1 1.1 Normal-order
C.S. 430 Assignment 6, Sample Solutions Paul Liu November 15, 2007 Note that these are sample solutions only; in many cases there were many acceptable answers. 1 Reynolds Problem 10.1 1.1 Normal-order
Modern Greek Extension
 Centre Number 2017 HIGHER SCHOOL CERTIFICATE EXAMINATION Student Number Modern Greek Extension Written Examination General Instructions Reading time 10 minutes Working time 1 hour and 50 minutes Write
Centre Number 2017 HIGHER SCHOOL CERTIFICATE EXAMINATION Student Number Modern Greek Extension Written Examination General Instructions Reading time 10 minutes Working time 1 hour and 50 minutes Write
Policy Coherence. JEL Classification : J12, J13, J21 Key words :
 ** 80%1.89 2005 7 35 Policy Coherence JEL Classification : J12, J13, J21 Key words : ** Family Life and Family Policy in France and Germany: Implications for Japan By Tomoko Hayashi and Rieko Tamefuji
** 80%1.89 2005 7 35 Policy Coherence JEL Classification : J12, J13, J21 Key words : ** Family Life and Family Policy in France and Germany: Implications for Japan By Tomoko Hayashi and Rieko Tamefuji
[1] P Q. Fig. 3.1
![[1] P Q. Fig. 3.1 [1] P Q. Fig. 3.1](/thumbs/79/80362156.jpg) 1 (a) Define resistance....... [1] (b) The smallest conductor within a computer processing chip can be represented as a rectangular block that is one atom high, four atoms wide and twenty atoms long. One
1 (a) Define resistance....... [1] (b) The smallest conductor within a computer processing chip can be represented as a rectangular block that is one atom high, four atoms wide and twenty atoms long. One
 Number All 397 Women 323 (81%) Men 74 (19%) Age(years) 39,1 (17-74) 38,9 (17-74) 40,5 (18-61) Maximum known weight(kg) 145,4 (92,0-292,0) 138,9 (92,0-202,0) 174,1 (126,0-292,0) Body mass index (kg/m 2
Number All 397 Women 323 (81%) Men 74 (19%) Age(years) 39,1 (17-74) 38,9 (17-74) 40,5 (18-61) Maximum known weight(kg) 145,4 (92,0-292,0) 138,9 (92,0-202,0) 174,1 (126,0-292,0) Body mass index (kg/m 2
Main source: "Discrete-time systems and computer control" by Α. ΣΚΟΔΡΑΣ ΨΗΦΙΑΚΟΣ ΕΛΕΓΧΟΣ ΔΙΑΛΕΞΗ 4 ΔΙΑΦΑΝΕΙΑ 1
 Main source: "Discrete-time systems and computer control" by Α. ΣΚΟΔΡΑΣ ΨΗΦΙΑΚΟΣ ΕΛΕΓΧΟΣ ΔΙΑΛΕΞΗ 4 ΔΙΑΦΑΝΕΙΑ 1 A Brief History of Sampling Research 1915 - Edmund Taylor Whittaker (1873-1956) devised a
Main source: "Discrete-time systems and computer control" by Α. ΣΚΟΔΡΑΣ ΨΗΦΙΑΚΟΣ ΕΛΕΓΧΟΣ ΔΙΑΛΕΞΗ 4 ΔΙΑΦΑΝΕΙΑ 1 A Brief History of Sampling Research 1915 - Edmund Taylor Whittaker (1873-1956) devised a
the total number of electrons passing through the lamp.
 1. A 12 V 36 W lamp is lit to normal brightness using a 12 V car battery of negligible internal resistance. The lamp is switched on for one hour (3600 s). For the time of 1 hour, calculate (i) the energy
1. A 12 V 36 W lamp is lit to normal brightness using a 12 V car battery of negligible internal resistance. The lamp is switched on for one hour (3600 s). For the time of 1 hour, calculate (i) the energy
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ ΤΜΗΜΑ ΝΟΣΗΛΕΥΤΙΚΗΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΕΠΗΡΕΑΖΕΙ ΤΗΝ ΠΡΟΛΗΨΗ ΚΑΡΚΙΝΟΥ ΤΟΥ ΜΑΣΤΟΥ
 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ ΤΜΗΜΑ ΝΟΣΗΛΕΥΤΙΚΗΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΠΩΣ Η ΚΑΤΑΝΑΛΩΣΗ ΦΡΟΥΤΩΝ ΚΑΙ ΛΑΧΑΝΙΚΩΝ ΕΠΗΡΕΑΖΕΙ ΤΗΝ ΠΡΟΛΗΨΗ ΚΑΡΚΙΝΟΥ ΤΟΥ ΜΑΣΤΟΥ Όνομα φοιτήτριας ΚΑΛΑΠΟΔΑ ΜΑΡΚΕΛΛΑ
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ ΤΜΗΜΑ ΝΟΣΗΛΕΥΤΙΚΗΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΠΩΣ Η ΚΑΤΑΝΑΛΩΣΗ ΦΡΟΥΤΩΝ ΚΑΙ ΛΑΧΑΝΙΚΩΝ ΕΠΗΡΕΑΖΕΙ ΤΗΝ ΠΡΟΛΗΨΗ ΚΑΡΚΙΝΟΥ ΤΟΥ ΜΑΣΤΟΥ Όνομα φοιτήτριας ΚΑΛΑΠΟΔΑ ΜΑΡΚΕΛΛΑ
Homework 3 Solutions
 Homework 3 Solutions Igor Yanovsky (Math 151A TA) Problem 1: Compute the absolute error and relative error in approximations of p by p. (Use calculator!) a) p π, p 22/7; b) p π, p 3.141. Solution: For
Homework 3 Solutions Igor Yanovsky (Math 151A TA) Problem 1: Compute the absolute error and relative error in approximations of p by p. (Use calculator!) a) p π, p 22/7; b) p π, p 3.141. Solution: For
Condition Behçet s syndrome. Behçet s syndrome. This booklet provides information and answers to your questions about this condition.
 Condition Behçet s syndrome This booklet provides information and answers to your questions about this condition. What is? is very rare in the UK only about 2,000 people have it. In this booklet we ll
Condition Behçet s syndrome This booklet provides information and answers to your questions about this condition. What is? is very rare in the UK only about 2,000 people have it. In this booklet we ll
Οι αδελφοί Montgolfier: Ψηφιακή αφήγηση The Montgolfier Βrothers Digital Story (προτείνεται να διδαχθεί στο Unit 4, Lesson 3, Αγγλικά Στ Δημοτικού)
 Οι αδελφοί Montgolfier: Ψηφιακή αφήγηση The Montgolfier Βrothers Digital Story (προτείνεται να διδαχθεί στο Unit 4, Lesson 3, Αγγλικά Στ Δημοτικού) Προσδοκώμενα αποτελέσματα Περιεχόμενο Ενδεικτικές δραστηριότητες
Οι αδελφοί Montgolfier: Ψηφιακή αφήγηση The Montgolfier Βrothers Digital Story (προτείνεται να διδαχθεί στο Unit 4, Lesson 3, Αγγλικά Στ Δημοτικού) Προσδοκώμενα αποτελέσματα Περιεχόμενο Ενδεικτικές δραστηριότητες
Section 7.6 Double and Half Angle Formulas
 09 Section 7. Double and Half Angle Fmulas To derive the double-angles fmulas, we will use the sum of two angles fmulas that we developed in the last section. We will let α θ and β θ: cos(θ) cos(θ + θ)
09 Section 7. Double and Half Angle Fmulas To derive the double-angles fmulas, we will use the sum of two angles fmulas that we developed in the last section. We will let α θ and β θ: cos(θ) cos(θ + θ)
b. Use the parametrization from (a) to compute the area of S a as S a ds. Be sure to substitute for ds!
 MTH U341 urface Integrals, tokes theorem, the divergence theorem To be turned in Wed., Dec. 1. 1. Let be the sphere of radius a, x 2 + y 2 + z 2 a 2. a. Use spherical coordinates (with ρ a) to parametrize.
MTH U341 urface Integrals, tokes theorem, the divergence theorem To be turned in Wed., Dec. 1. 1. Let be the sphere of radius a, x 2 + y 2 + z 2 a 2. a. Use spherical coordinates (with ρ a) to parametrize.
Πτυχιακή Εργασία Η ΠΟΙΟΤΗΤΑ ΖΩΗΣ ΤΩΝ ΑΣΘΕΝΩΝ ΜΕ ΣΤΗΘΑΓΧΗ
 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ Πτυχιακή Εργασία Η ΠΟΙΟΤΗΤΑ ΖΩΗΣ ΤΩΝ ΑΣΘΕΝΩΝ ΜΕ ΣΤΗΘΑΓΧΗ Νικόλας Χριστοδούλου Λευκωσία, 2012 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ Πτυχιακή Εργασία Η ΠΟΙΟΤΗΤΑ ΖΩΗΣ ΤΩΝ ΑΣΘΕΝΩΝ ΜΕ ΣΤΗΘΑΓΧΗ Νικόλας Χριστοδούλου Λευκωσία, 2012 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ
ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΠΛΗΡΟΦΟΡΙΚΗΣ CYPRUS COMPUTER SOCIETY ΠΑΓΚΥΠΡΙΟΣ ΜΑΘΗΤΙΚΟΣ ΔΙΑΓΩΝΙΣΜΟΣ ΠΛΗΡΟΦΟΡΙΚΗΣ 6/5/2006
 Οδηγίες: Να απαντηθούν όλες οι ερωτήσεις. Ολοι οι αριθμοί που αναφέρονται σε όλα τα ερωτήματα είναι μικρότεροι το 1000 εκτός αν ορίζεται διαφορετικά στη διατύπωση του προβλήματος. Διάρκεια: 3,5 ώρες Καλή
Οδηγίες: Να απαντηθούν όλες οι ερωτήσεις. Ολοι οι αριθμοί που αναφέρονται σε όλα τα ερωτήματα είναι μικρότεροι το 1000 εκτός αν ορίζεται διαφορετικά στη διατύπωση του προβλήματος. Διάρκεια: 3,5 ώρες Καλή
Paper Reference. Paper Reference(s) 1776/04 Edexcel GCSE Modern Greek Paper 4 Writing. Thursday 21 May 2009 Afternoon Time: 1 hour 15 minutes
 Centre No. Candidate No. Paper Reference(s) 1776/04 Edexcel GCSE Modern Greek Paper 4 Writing Thursday 21 May 2009 Afternoon Time: 1 hour 15 minutes Materials required for examination Nil Paper Reference
Centre No. Candidate No. Paper Reference(s) 1776/04 Edexcel GCSE Modern Greek Paper 4 Writing Thursday 21 May 2009 Afternoon Time: 1 hour 15 minutes Materials required for examination Nil Paper Reference
PARTIAL NOTES for 6.1 Trigonometric Identities
 PARTIAL NOTES for 6.1 Trigonometric Identities tanθ = sinθ cosθ cotθ = cosθ sinθ BASIC IDENTITIES cscθ = 1 sinθ secθ = 1 cosθ cotθ = 1 tanθ PYTHAGOREAN IDENTITIES sin θ + cos θ =1 tan θ +1= sec θ 1 + cot
PARTIAL NOTES for 6.1 Trigonometric Identities tanθ = sinθ cosθ cotθ = cosθ sinθ BASIC IDENTITIES cscθ = 1 sinθ secθ = 1 cosθ cotθ = 1 tanθ PYTHAGOREAN IDENTITIES sin θ + cos θ =1 tan θ +1= sec θ 1 + cot
ΠΕΡΙΛΗΨΗ. Εισαγωγή. Σκοπός
 ΠΕΡΙΛΗΨΗ Εισαγωγή Η παιδική παχυσαρκία έχει φτάσει σε επίπεδα επιδημίας στις μέρες μας. Μαστίζει παιδιά από μικρές ηλικίες μέχρι και σε εφήβους. Συντείνουν αρκετοί παράγοντες που ένα παιδί γίνεται παχύσαρκο
ΠΕΡΙΛΗΨΗ Εισαγωγή Η παιδική παχυσαρκία έχει φτάσει σε επίπεδα επιδημίας στις μέρες μας. Μαστίζει παιδιά από μικρές ηλικίες μέχρι και σε εφήβους. Συντείνουν αρκετοί παράγοντες που ένα παιδί γίνεται παχύσαρκο
ΑΓΓΛΙΚΗ ΓΛΩΣΣΑ ΣΕ ΕΙΔΙΚΑ ΘΕΜΑΤΑ ΔΙΕΘΝΩΝ ΣΧΕΣΕΩΝ & ΟΙΚΟΝΟΜΙΑΣ
 ΑΓΓΛΙΚΗ ΓΛΩΣΣΑ ΣΕ ΕΙΔΙΚΑ ΘΕΜΑΤΑ ΔΙΕΘΝΩΝ ΣΧΕΣΕΩΝ & ΟΙΚΟΝΟΜΙΑΣ Ενότητα 3β: Types of Speeches & Strong Language Ιφιγένεια Μαχίλη Άδειες Χρήσης Το παρόν εκπαιδευτικό υλικό υπόκειται σε άδειες χρήσης Creative
ΑΓΓΛΙΚΗ ΓΛΩΣΣΑ ΣΕ ΕΙΔΙΚΑ ΘΕΜΑΤΑ ΔΙΕΘΝΩΝ ΣΧΕΣΕΩΝ & ΟΙΚΟΝΟΜΙΑΣ Ενότητα 3β: Types of Speeches & Strong Language Ιφιγένεια Μαχίλη Άδειες Χρήσης Το παρόν εκπαιδευτικό υλικό υπόκειται σε άδειες χρήσης Creative
5.4 The Poisson Distribution.
 The worst thing you can do about a situation is nothing. Sr. O Shea Jackson 5.4 The Poisson Distribution. Description of the Poisson Distribution Discrete probability distribution. The random variable
The worst thing you can do about a situation is nothing. Sr. O Shea Jackson 5.4 The Poisson Distribution. Description of the Poisson Distribution Discrete probability distribution. The random variable
Section 9.2 Polar Equations and Graphs
 180 Section 9. Polar Equations and Graphs In this section, we will be graphing polar equations on a polar grid. In the first few examples, we will write the polar equation in rectangular form to help identify
180 Section 9. Polar Equations and Graphs In this section, we will be graphing polar equations on a polar grid. In the first few examples, we will write the polar equation in rectangular form to help identify
Advanced Subsidiary Unit 1: Understanding and Written Response
 Write your name here Surname Other names Edexcel GE entre Number andidate Number Greek dvanced Subsidiary Unit 1: Understanding and Written Response Thursday 16 May 2013 Morning Time: 2 hours 45 minutes
Write your name here Surname Other names Edexcel GE entre Number andidate Number Greek dvanced Subsidiary Unit 1: Understanding and Written Response Thursday 16 May 2013 Morning Time: 2 hours 45 minutes
ΟΙΚΟΝΟΜΟΤΕΧΝΙΚΗ ΑΝΑΛΥΣΗ ΕΝΟΣ ΕΝΕΡΓΕΙΑΚΑ ΑΥΤΟΝΟΜΟΥ ΝΗΣΙΟΥ ΜΕ Α.Π.Ε
 Τμήμα Ηλεκτρονικών Μηχανικών Τ.Ε. ΟΙΚΟΝΟΜΟΤΕΧΝΙΚΗ ΑΝΑΛΥΣΗ ΕΝΟΣ ΕΝΕΡΓΕΙΑΚΑ ΑΥΤΟΝΟΜΟΥ ΝΗΣΙΟΥ ΜΕ Α.Π.Ε Πτυχιακή Εργασία Φοιτητής: Γεμενής Κωνσταντίνος ΑΜ: 30931 Επιβλέπων Καθηγητής Κοκκόσης Απόστολος Λέκτορας
Τμήμα Ηλεκτρονικών Μηχανικών Τ.Ε. ΟΙΚΟΝΟΜΟΤΕΧΝΙΚΗ ΑΝΑΛΥΣΗ ΕΝΟΣ ΕΝΕΡΓΕΙΑΚΑ ΑΥΤΟΝΟΜΟΥ ΝΗΣΙΟΥ ΜΕ Α.Π.Ε Πτυχιακή Εργασία Φοιτητής: Γεμενής Κωνσταντίνος ΑΜ: 30931 Επιβλέπων Καθηγητής Κοκκόσης Απόστολος Λέκτορας
Group 2 Methotrexate 7.5 mg/week, increased to 15 mg/week after 4 weeks. Methotrexate 7.5 mg/week, increased to 15 mg/week after 4 weeks
 Group 1 Methotrexate 7.5 mg/week, increased to 15 mg/week after 4 weeks Group 2 Methotrexate 7.5 mg/week, increased to 15 mg/week after 4 weeks Sulfasalazine 2000-3000 mg/day Leflunomide 20 mg/day Infliximab
Group 1 Methotrexate 7.5 mg/week, increased to 15 mg/week after 4 weeks Group 2 Methotrexate 7.5 mg/week, increased to 15 mg/week after 4 weeks Sulfasalazine 2000-3000 mg/day Leflunomide 20 mg/day Infliximab
Απόκριση σε Μοναδιαία Ωστική Δύναμη (Unit Impulse) Απόκριση σε Δυνάμεις Αυθαίρετα Μεταβαλλόμενες με το Χρόνο. Απόστολος Σ.
 Απόκριση σε Δυνάμεις Αυθαίρετα Μεταβαλλόμενες με το Χρόνο The time integral of a force is referred to as impulse, is determined by and is obtained from: Newton s 2 nd Law of motion states that the action
Απόκριση σε Δυνάμεις Αυθαίρετα Μεταβαλλόμενες με το Χρόνο The time integral of a force is referred to as impulse, is determined by and is obtained from: Newton s 2 nd Law of motion states that the action
3.4 SUM AND DIFFERENCE FORMULAS. NOTE: cos(α+β) cos α + cos β cos(α-β) cos α -cos β
 3.4 SUM AND DIFFERENCE FORMULAS Page Theorem cos(αβ cos α cos β -sin α cos(α-β cos α cos β sin α NOTE: cos(αβ cos α cos β cos(α-β cos α -cos β Proof of cos(α-β cos α cos β sin α Let s use a unit circle
3.4 SUM AND DIFFERENCE FORMULAS Page Theorem cos(αβ cos α cos β -sin α cos(α-β cos α cos β sin α NOTE: cos(αβ cos α cos β cos(α-β cos α -cos β Proof of cos(α-β cos α cos β sin α Let s use a unit circle
CHAPTER 25 SOLVING EQUATIONS BY ITERATIVE METHODS
 CHAPTER 5 SOLVING EQUATIONS BY ITERATIVE METHODS EXERCISE 104 Page 8 1. Find the positive root of the equation x + 3x 5 = 0, correct to 3 significant figures, using the method of bisection. Let f(x) =
CHAPTER 5 SOLVING EQUATIONS BY ITERATIVE METHODS EXERCISE 104 Page 8 1. Find the positive root of the equation x + 3x 5 = 0, correct to 3 significant figures, using the method of bisection. Let f(x) =
Capacitors - Capacitance, Charge and Potential Difference
 Capacitors - Capacitance, Charge and Potential Difference Capacitors store electric charge. This ability to store electric charge is known as capacitance. A simple capacitor consists of 2 parallel metal
Capacitors - Capacitance, Charge and Potential Difference Capacitors store electric charge. This ability to store electric charge is known as capacitance. A simple capacitor consists of 2 parallel metal
ίκτυο προστασίας για τα Ελληνικά αγροτικά και οικόσιτα ζώα on.net e-foundatio //www.save itute: http:/ toring Insti SAVE-Monit
 How to run a Herdbook: Basics and Basics According to the pedigree scheme, you need to write down the ancestors of your animals. Breeders should be able easily to write down the necessary data It is better
How to run a Herdbook: Basics and Basics According to the pedigree scheme, you need to write down the ancestors of your animals. Breeders should be able easily to write down the necessary data It is better
TMA4115 Matematikk 3
 TMA4115 Matematikk 3 Andrew Stacey Norges Teknisk-Naturvitenskapelige Universitet Trondheim Spring 2010 Lecture 12: Mathematics Marvellous Matrices Andrew Stacey Norges Teknisk-Naturvitenskapelige Universitet
TMA4115 Matematikk 3 Andrew Stacey Norges Teknisk-Naturvitenskapelige Universitet Trondheim Spring 2010 Lecture 12: Mathematics Marvellous Matrices Andrew Stacey Norges Teknisk-Naturvitenskapelige Universitet
department listing department name αχχουντσ ϕανε βαλικτ δδσϕηασδδη σδηφγ ασκϕηλκ τεχηνιχαλ αλαν ϕουν διξ τεχηνιχαλ ϕοην µαριανι
 She selects the option. Jenny starts with the al listing. This has employees listed within She drills down through the employee. The inferred ER sttricture relates this to the redcords in the databasee
She selects the option. Jenny starts with the al listing. This has employees listed within She drills down through the employee. The inferred ER sttricture relates this to the redcords in the databasee
Mean bond enthalpy Standard enthalpy of formation Bond N H N N N N H O O O
 Q1. (a) Explain the meaning of the terms mean bond enthalpy and standard enthalpy of formation. Mean bond enthalpy... Standard enthalpy of formation... (5) (b) Some mean bond enthalpies are given below.
Q1. (a) Explain the meaning of the terms mean bond enthalpy and standard enthalpy of formation. Mean bond enthalpy... Standard enthalpy of formation... (5) (b) Some mean bond enthalpies are given below.
Χρειάζεται να φέρω μαζί μου τα πρωτότυπα έγγραφα ή τα αντίγραφα; Asking if you need to provide the original documents or copies Ποια είναι τα κριτήρια
 - University Θα ήθελα να εγγραφώ σε πανεπιστήμιο. Stating that you want to enroll Θα ήθελα να γραφτώ για. Stating that you want to apply for a course ένα προπτυχιακό ένα μεταπτυχιακό ένα διδακτορικό πλήρους
- University Θα ήθελα να εγγραφώ σε πανεπιστήμιο. Stating that you want to enroll Θα ήθελα να γραφτώ για. Stating that you want to apply for a course ένα προπτυχιακό ένα μεταπτυχιακό ένα διδακτορικό πλήρους
ΙΑΤΡΟΦΙΚΗ ΦΡΟΝΤΙ Α ΓΙΑ ΤΑΞΙ ΙΩΤΕΣ ΣΥΝΤΟΜΗΣ ΚΑΙ ΜΑΚΡΑΣ ΙΑΡΚΕΙΑΣ
 ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΤΜΗΜΑ ΙΑΤΡΟΦΗΣ ΚΑΙ ΙΑΙΤΟΛΟΓΙΑΣ, ΤΕΙ ΚΡΗΤΗΣ ΙΑΤΡΟΦΙΚΗ ΦΡΟΝΤΙ Α ΓΙΑ ΤΑΞΙ ΙΩΤΕΣ ΣΥΝΤΟΜΗΣ ΚΑΙ ΜΑΚΡΑΣ ΙΑΡΚΕΙΑΣ ΕΠΙΜΕΛΕΙΑ: ΑΛΕΞΙΑ ΤΣΕΡΛΙΓΚΑ ΥΠΕΥΘΥΝΟΣ ΚΑΘΗΓΗΤΗΣ: Γ. Α. ΦΡΑΓΚΙΑ ΑΚΗΣ. 2012 σελ.
ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΤΜΗΜΑ ΙΑΤΡΟΦΗΣ ΚΑΙ ΙΑΙΤΟΛΟΓΙΑΣ, ΤΕΙ ΚΡΗΤΗΣ ΙΑΤΡΟΦΙΚΗ ΦΡΟΝΤΙ Α ΓΙΑ ΤΑΞΙ ΙΩΤΕΣ ΣΥΝΤΟΜΗΣ ΚΑΙ ΜΑΚΡΑΣ ΙΑΡΚΕΙΑΣ ΕΠΙΜΕΛΕΙΑ: ΑΛΕΞΙΑ ΤΣΕΡΛΙΓΚΑ ΥΠΕΥΘΥΝΟΣ ΚΑΘΗΓΗΤΗΣ: Γ. Α. ΦΡΑΓΚΙΑ ΑΚΗΣ. 2012 σελ.
ΣΟΡΟΠΤΙΜΙΣΤΡΙΕΣ ΕΛΛΗΝΙΔΕΣ
 ΕΛΛΗΝΙΔΕΣ ΣΟΡΟΠΤΙΜΙΣΤΡΙΕΣ ΕΚΔΟΣΗ ΤΗΣ ΣΟΡΟΠΤΙΜΙΣΤΙΚΗΣ ΕΝΩΣΗΣ ΕΛΛΑΔΟΣ - ΤΕΥΧΟΣ Νο 110 - Δ ΤΡΙΜΗΝΟ 2014 Το πρώτο βραβείο κέρδισε η Ελλάδα για την φωτογραφία Blue + Yellow = Green στον διαγωνισμό 2014 του
ΕΛΛΗΝΙΔΕΣ ΣΟΡΟΠΤΙΜΙΣΤΡΙΕΣ ΕΚΔΟΣΗ ΤΗΣ ΣΟΡΟΠΤΙΜΙΣΤΙΚΗΣ ΕΝΩΣΗΣ ΕΛΛΑΔΟΣ - ΤΕΥΧΟΣ Νο 110 - Δ ΤΡΙΜΗΝΟ 2014 Το πρώτο βραβείο κέρδισε η Ελλάδα για την φωτογραφία Blue + Yellow = Green στον διαγωνισμό 2014 του
Section 1: Listening and responding. Presenter: Niki Farfara MGTAV VCE Seminar 7 August 2016
 Section 1: Listening and responding Presenter: Niki Farfara MGTAV VCE Seminar 7 August 2016 Section 1: Listening and responding Section 1: Listening and Responding/ Aκουστική εξέταση Στο πρώτο μέρος της
Section 1: Listening and responding Presenter: Niki Farfara MGTAV VCE Seminar 7 August 2016 Section 1: Listening and responding Section 1: Listening and Responding/ Aκουστική εξέταση Στο πρώτο μέρος της
Concrete Mathematics Exercises from 30 September 2016
 Concrete Mathematics Exercises from 30 September 2016 Silvio Capobianco Exercise 1.7 Let H(n) = J(n + 1) J(n). Equation (1.8) tells us that H(2n) = 2, and H(2n+1) = J(2n+2) J(2n+1) = (2J(n+1) 1) (2J(n)+1)
Concrete Mathematics Exercises from 30 September 2016 Silvio Capobianco Exercise 1.7 Let H(n) = J(n + 1) J(n). Equation (1.8) tells us that H(2n) = 2, and H(2n+1) = J(2n+2) J(2n+1) = (2J(n+1) 1) (2J(n)+1)
Ελληνικά/Αγγλικά Greek/English. Κατανοώντας τη. Νόσο του Πάρκινσον. Understanding. Parkinson s disease. Parkinson s Australia
 Ελληνικά/Αγγλικά Greek/English Κατανοώντας τη Νόσο του Πάρκινσον Understanding Parkinson s disease Parkinson s What is Parkinson s disease? Tι είναι η νόσος του Πάρκινσον; Parkinson s disease is a condition
Ελληνικά/Αγγλικά Greek/English Κατανοώντας τη Νόσο του Πάρκινσον Understanding Parkinson s disease Parkinson s What is Parkinson s disease? Tι είναι η νόσος του Πάρκινσον; Parkinson s disease is a condition
Επιβλέπων καθηγητής: Δρ Βασίλειος Ραφτόπουλος ΠΟΙΟΤΗΤΑ ΖΩΗΣ ΣΕ ΜΕΤΕΜΜΗΝΟΠΑΥΣΙΑΚΕΣ ΓΥΝΑΙΚΕΣ ΜΕΤΑ ΑΠΟ ΟΣΤΕΟΠΟΡΩΤΙΚΑ ΚΑΤΑΓΜΑΤΑ ΣΠΟΝΔΥΛΙΚΗΣ ΣΤΗΛΗΣ
 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΤΜΗΜΑ ΝΟΣΗΛΕΥΤΙΚΗΣ Επιβλέπων καθηγητής: Δρ Βασίλειος Ραφτόπουλος ΠΟΙΟΤΗΤΑ ΖΩΗΣ ΣΕ ΜΕΤΕΜΜΗΝΟΠΑΥΣΙΑΚΕΣ ΓΥΝΑΙΚΕΣ ΜΕΤΑ ΑΠΟ ΟΣΤΕΟΠΟΡΩΤΙΚΑ ΚΑΤΑΓΜΑΤΑ ΣΠΟΝΔΥΛΙΚΗΣ ΣΤΗΛΗΣ Από τη
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΤΜΗΜΑ ΝΟΣΗΛΕΥΤΙΚΗΣ Επιβλέπων καθηγητής: Δρ Βασίλειος Ραφτόπουλος ΠΟΙΟΤΗΤΑ ΖΩΗΣ ΣΕ ΜΕΤΕΜΜΗΝΟΠΑΥΣΙΑΚΕΣ ΓΥΝΑΙΚΕΣ ΜΕΤΑ ΑΠΟ ΟΣΤΕΟΠΟΡΩΤΙΚΑ ΚΑΤΑΓΜΑΤΑ ΣΠΟΝΔΥΛΙΚΗΣ ΣΤΗΛΗΣ Από τη
Math 6 SL Probability Distributions Practice Test Mark Scheme
 Math 6 SL Probability Distributions Practice Test Mark Scheme. (a) Note: Award A for vertical line to right of mean, A for shading to right of their vertical line. AA N (b) evidence of recognizing symmetry
Math 6 SL Probability Distributions Practice Test Mark Scheme. (a) Note: Award A for vertical line to right of mean, A for shading to right of their vertical line. AA N (b) evidence of recognizing symmetry
ΓΕΩΠΟΝΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΑΘΗΝΩΝ ΤΜΗΜΑ ΕΠΙΣΤΗΜΗΣ ΤΡΟΦΙΜΩΝ ΚΑΙ ΔΙΑΤΡΟΦΗΣ ΤΟΥ ΑΝΘΡΩΠΟΥ
 ΓΕΩΠΟΝΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΑΘΗΝΩΝ ΤΜΗΜΑ ΕΠΙΣΤΗΜΗΣ ΤΡΟΦΙΜΩΝ ΚΑΙ ΔΙΑΤΡΟΦΗΣ ΤΟΥ ΑΝΘΡΩΠΟΥ Πρόγραμμα Μεταπτυχιακών Σπουδών «Επιστήμη και Τεχνολογία Τροφίμων και Διατροφή του Ανθρώπου» Κατεύθυνση: «Διατροφή, Δημόσια
ΓΕΩΠΟΝΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΑΘΗΝΩΝ ΤΜΗΜΑ ΕΠΙΣΤΗΜΗΣ ΤΡΟΦΙΜΩΝ ΚΑΙ ΔΙΑΤΡΟΦΗΣ ΤΟΥ ΑΝΘΡΩΠΟΥ Πρόγραμμα Μεταπτυχιακών Σπουδών «Επιστήμη και Τεχνολογία Τροφίμων και Διατροφή του Ανθρώπου» Κατεύθυνση: «Διατροφή, Δημόσια
BECAUSE WE REALLY WANT TO KNOW WHAT YOU THINK ABOUT SCHOOL AND YOUR GARDEN. Fairly true If I decide to learn something hard, I can.
 BECAUSE WE REALLY WANT TO KNOW WHAT YOU THINK ABOUT SCHOOL AND YOUR GARDEN Name GRADE Science Teacher A. What do I think about School? bit I try hard to do well in school. I look forward to coming to school.
BECAUSE WE REALLY WANT TO KNOW WHAT YOU THINK ABOUT SCHOOL AND YOUR GARDEN Name GRADE Science Teacher A. What do I think about School? bit I try hard to do well in school. I look forward to coming to school.
ΠΑΝΕΠΙΣΤΗΜΙΟ ΠΑΤΡΩΝ ΤΜΗΜΑ ΗΛΕΚΤΡΟΛΟΓΩΝ ΜΗΧΑΝΙΚΩΝ ΚΑΙ ΤΕΧΝΟΛΟΓΙΑΣ ΥΠΟΛΟΓΙΣΤΩΝ ΤΟΜΕΑΣ ΣΥΣΤΗΜΑΤΩΝ ΗΛΕΚΤΡΙΚΗΣ ΕΝΕΡΓΕΙΑΣ
 ΠΑΝΕΠΙΣΤΗΜΙΟ ΠΑΤΡΩΝ ΤΜΗΜΑ ΗΛΕΚΤΡΟΛΟΓΩΝ ΜΗΧΑΝΙΚΩΝ ΚΑΙ ΤΕΧΝΟΛΟΓΙΑΣ ΥΠΟΛΟΓΙΣΤΩΝ ΤΟΜΕΑΣ ΣΥΣΤΗΜΑΤΩΝ ΗΛΕΚΤΡΙΚΗΣ ΕΝΕΡΓΕΙΑΣ ιπλωµατική Εργασία του φοιτητή του τµήµατος Ηλεκτρολόγων Μηχανικών και Τεχνολογίας Ηλεκτρονικών
ΠΑΝΕΠΙΣΤΗΜΙΟ ΠΑΤΡΩΝ ΤΜΗΜΑ ΗΛΕΚΤΡΟΛΟΓΩΝ ΜΗΧΑΝΙΚΩΝ ΚΑΙ ΤΕΧΝΟΛΟΓΙΑΣ ΥΠΟΛΟΓΙΣΤΩΝ ΤΟΜΕΑΣ ΣΥΣΤΗΜΑΤΩΝ ΗΛΕΚΤΡΙΚΗΣ ΕΝΕΡΓΕΙΑΣ ιπλωµατική Εργασία του φοιτητή του τµήµατος Ηλεκτρολόγων Μηχανικών και Τεχνολογίας Ηλεκτρονικών
Συστήματα Διαχείρισης Βάσεων Δεδομένων
 ΕΛΛΗΝΙΚΗ ΔΗΜΟΚΡΑΤΙΑ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΡΗΤΗΣ Συστήματα Διαχείρισης Βάσεων Δεδομένων Φροντιστήριο 9: Transactions - part 1 Δημήτρης Πλεξουσάκης Τμήμα Επιστήμης Υπολογιστών Tutorial on Undo, Redo and Undo/Redo
ΕΛΛΗΝΙΚΗ ΔΗΜΟΚΡΑΤΙΑ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΡΗΤΗΣ Συστήματα Διαχείρισης Βάσεων Δεδομένων Φροντιστήριο 9: Transactions - part 1 Δημήτρης Πλεξουσάκης Τμήμα Επιστήμης Υπολογιστών Tutorial on Undo, Redo and Undo/Redo
Calculating the propagation delay of coaxial cable
 Your source for quality GNSS Networking Solutions and Design Services! Page 1 of 5 Calculating the propagation delay of coaxial cable The delay of a cable or velocity factor is determined by the dielectric
Your source for quality GNSS Networking Solutions and Design Services! Page 1 of 5 Calculating the propagation delay of coaxial cable The delay of a cable or velocity factor is determined by the dielectric
Ακαδημαϊκός Λόγος Εισαγωγή
 - In this essay/paper/thesis I shall examine/investigate/evaluate/analyze Γενική εισαγωγή για μια εργασία/διατριβή Σε αυτήν την εργασία/διατριβή θα αναλύσω/εξετάσω/διερευνήσω/αξιολογήσω... To answer this
- In this essay/paper/thesis I shall examine/investigate/evaluate/analyze Γενική εισαγωγή για μια εργασία/διατριβή Σε αυτήν την εργασία/διατριβή θα αναλύσω/εξετάσω/διερευνήσω/αξιολογήσω... To answer this
Condition Gout. Gout. This booklet provides information and answers to your questions about this condition.
 Condition This booklet provides information and answers to your questions about this condition. What is gout? is often said to be the most painful form of arthritis. In this booklet we ll explain what
Condition This booklet provides information and answers to your questions about this condition. What is gout? is often said to be the most painful form of arthritis. In this booklet we ll explain what
Antiphospholipid syndrome (APS)
 Condition Antiphospholipid syndrome (APS) Antiphospholipid syndrome (APS) This booklet provides information and answers to your questions about this condition. What is antiphospholipid syndrome (APS)?
Condition Antiphospholipid syndrome (APS) Antiphospholipid syndrome (APS) This booklet provides information and answers to your questions about this condition. What is antiphospholipid syndrome (APS)?
Writing for A class. Describe yourself Topic 1: Write your name, your nationality, your hobby, your pet. Write where you live.
 Topic 1: Describe yourself Write your name, your nationality, your hobby, your pet. Write where you live. Χρησιμοποίησε το and. WRITE your paragraph in 40-60 words... 1 Topic 2: Describe your room Χρησιμοποίησε
Topic 1: Describe yourself Write your name, your nationality, your hobby, your pet. Write where you live. Χρησιμοποίησε το and. WRITE your paragraph in 40-60 words... 1 Topic 2: Describe your room Χρησιμοποίησε
Potential Dividers. 46 minutes. 46 marks. Page 1 of 11
 Potential Dividers 46 minutes 46 marks Page 1 of 11 Q1. In the circuit shown in the figure below, the battery, of negligible internal resistance, has an emf of 30 V. The pd across the lamp is 6.0 V and
Potential Dividers 46 minutes 46 marks Page 1 of 11 Q1. In the circuit shown in the figure below, the battery, of negligible internal resistance, has an emf of 30 V. The pd across the lamp is 6.0 V and
Μηχανική Μάθηση Hypothesis Testing
 ΕΛΛΗΝΙΚΗ ΔΗΜΟΚΡΑΤΙΑ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΡΗΤΗΣ Μηχανική Μάθηση Hypothesis Testing Γιώργος Μπορμπουδάκης Τμήμα Επιστήμης Υπολογιστών Procedure 1. Form the null (H 0 ) and alternative (H 1 ) hypothesis 2. Consider
ΕΛΛΗΝΙΚΗ ΔΗΜΟΚΡΑΤΙΑ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΡΗΤΗΣ Μηχανική Μάθηση Hypothesis Testing Γιώργος Μπορμπουδάκης Τμήμα Επιστήμης Υπολογιστών Procedure 1. Form the null (H 0 ) and alternative (H 1 ) hypothesis 2. Consider
ΚΑΠΝΙΣΜΑ ΚΑΙ ΣΥΝΔΡΟΜΟ ΑΙΦΝΙΔΙΟΥ ΒΡΕΦΙΚΟΥ ΘΑΝΑΤΟΥ
 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΚΑΠΝΙΣΜΑ ΚΑΙ ΣΥΝΔΡΟΜΟ ΑΙΦΝΙΔΙΟΥ ΒΡΕΦΙΚΟΥ ΘΑΝΑΤΟΥ Ονοματεπώνυμο: Λοϊζιά Ελένη Λεμεσός 2012 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΚΑΠΝΙΣΜΑ ΚΑΙ ΣΥΝΔΡΟΜΟ ΑΙΦΝΙΔΙΟΥ ΒΡΕΦΙΚΟΥ ΘΑΝΑΤΟΥ Ονοματεπώνυμο: Λοϊζιά Ελένη Λεμεσός 2012 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ
ΚΥΠΡΙΑΚΟΣ ΣΥΝΔΕΣΜΟΣ ΠΛΗΡΟΦΟΡΙΚΗΣ CYPRUS COMPUTER SOCIETY 21 ος ΠΑΓΚΥΠΡΙΟΣ ΜΑΘΗΤΙΚΟΣ ΔΙΑΓΩΝΙΣΜΟΣ ΠΛΗΡΟΦΟΡΙΚΗΣ Δεύτερος Γύρος - 30 Μαρτίου 2011
 Διάρκεια Διαγωνισμού: 3 ώρες Απαντήστε όλες τις ερωτήσεις Μέγιστο Βάρος (20 Μονάδες) Δίνεται ένα σύνολο από N σφαιρίδια τα οποία δεν έχουν όλα το ίδιο βάρος μεταξύ τους και ένα κουτί που αντέχει μέχρι
Διάρκεια Διαγωνισμού: 3 ώρες Απαντήστε όλες τις ερωτήσεις Μέγιστο Βάρος (20 Μονάδες) Δίνεται ένα σύνολο από N σφαιρίδια τα οποία δεν έχουν όλα το ίδιο βάρος μεταξύ τους και ένα κουτί που αντέχει μέχρι
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ
 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΑΞΙΟΛΟΓΗΣΗ ΣΤΑΣΕΩΝ ΚΑΙ ΕΠΙΠΕΔΟΥ ΓΝΩΣΕΩΝ ΤΩΝ ΝΟΣΗΛΕΥΤΩΝ ΣΕ ΜΟΝΑΔΕΣ ΕΝΤΑΤΙΚΗΣ ΘΕΡΑΠΕΙΑΣ ΣΧΕΤΙΚΑ ΜΕ ΤΗ ΜΕΤΑΜΟΣΧΕΥΣΗ ΟΡΓΑΝΩΝ ΑΠΟ ΕΓΚΕΦΑΛΙΚΑ
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ ΠΤΥΧΙΑΚΗ ΕΡΓΑΣΙΑ ΑΞΙΟΛΟΓΗΣΗ ΣΤΑΣΕΩΝ ΚΑΙ ΕΠΙΠΕΔΟΥ ΓΝΩΣΕΩΝ ΤΩΝ ΝΟΣΗΛΕΥΤΩΝ ΣΕ ΜΟΝΑΔΕΣ ΕΝΤΑΤΙΚΗΣ ΘΕΡΑΠΕΙΑΣ ΣΧΕΤΙΚΑ ΜΕ ΤΗ ΜΕΤΑΜΟΣΧΕΥΣΗ ΟΡΓΑΝΩΝ ΑΠΟ ΕΓΚΕΦΑΛΙΚΑ
Condition Reactive arthritis. Reactive arthritis. This booklet provides information and answers to your questions about this condition.
 Condition This booklet provides information and answers to your questions about this condition. What is reactive arthritis? is a condition which can develop following an infection of the bowel or genital
Condition This booklet provides information and answers to your questions about this condition. What is reactive arthritis? is a condition which can develop following an infection of the bowel or genital
HIV HIV HIV HIV AIDS 3 :.1 /-,**1 +332
 ,**1 The Japanese Society for AIDS Research The Journal of AIDS Research +,, +,, +,, + -. / 0 1 +, -. / 0 1 : :,**- +,**. 1..+ - : +** 22 HIV AIDS HIV HIV AIDS : HIV AIDS HIV :HIV AIDS 3 :.1 /-,**1 HIV
,**1 The Japanese Society for AIDS Research The Journal of AIDS Research +,, +,, +,, + -. / 0 1 +, -. / 0 1 : :,**- +,**. 1..+ - : +** 22 HIV AIDS HIV HIV AIDS : HIV AIDS HIV :HIV AIDS 3 :.1 /-,**1 HIV
Strain gauge and rosettes
 Strain gauge and rosettes Introduction A strain gauge is a device which is used to measure strain (deformation) on an object subjected to forces. Strain can be measured using various types of devices classified
Strain gauge and rosettes Introduction A strain gauge is a device which is used to measure strain (deformation) on an object subjected to forces. Strain can be measured using various types of devices classified
Ακαδημαϊκός Λόγος Εισαγωγή
 - Σε αυτήν την εργασία/διατριβή θα αναλύσω/εξετάσω/διερευνήσω/αξιολογήσω... Γενική εισαγωγή για μια εργασία/διατριβή In this essay/paper/thesis I shall examine/investigate/evaluate/analyze Για να απαντήσουμε
- Σε αυτήν την εργασία/διατριβή θα αναλύσω/εξετάσω/διερευνήσω/αξιολογήσω... Γενική εισαγωγή για μια εργασία/διατριβή In this essay/paper/thesis I shall examine/investigate/evaluate/analyze Για να απαντήσουμε
ΠΑΡΑΜΕΤΡΟΙ ΕΠΗΡΕΑΣΜΟΥ ΤΗΣ ΑΝΑΓΝΩΣΗΣ- ΑΠΟΚΩΔΙΚΟΠΟΙΗΣΗΣ ΤΗΣ BRAILLE ΑΠΟ ΑΤΟΜΑ ΜΕ ΤΥΦΛΩΣΗ
 ΠΑΝΕΠΙΣΤΗΜΙΟ ΜΑΚΕΔΟΝΙΑΣ ΟΙΚΟΝΟΜΙΚΩΝ ΚΑΙ ΚΟΙΝΩΝΙΚΩΝ ΕΠΙΣΤΗΜΩΝ ΤΜΗΜΑ ΕΚΠΑΙΔΕΥΤΙΚΗΣ ΚΑΙ ΚΟΙΝΩΝΙΚΗΣ ΠΟΛΙΤΙΚΗΣ ΠΡΟΓΡΑΜΜΑ ΜΕΤΑΠΤΥΧΙΑΚΩΝ ΣΠΟΥΔΩΝ ΠΑΡΑΜΕΤΡΟΙ ΕΠΗΡΕΑΣΜΟΥ ΤΗΣ ΑΝΑΓΝΩΣΗΣ- ΑΠΟΚΩΔΙΚΟΠΟΙΗΣΗΣ ΤΗΣ BRAILLE
ΠΑΝΕΠΙΣΤΗΜΙΟ ΜΑΚΕΔΟΝΙΑΣ ΟΙΚΟΝΟΜΙΚΩΝ ΚΑΙ ΚΟΙΝΩΝΙΚΩΝ ΕΠΙΣΤΗΜΩΝ ΤΜΗΜΑ ΕΚΠΑΙΔΕΥΤΙΚΗΣ ΚΑΙ ΚΟΙΝΩΝΙΚΗΣ ΠΟΛΙΤΙΚΗΣ ΠΡΟΓΡΑΜΜΑ ΜΕΤΑΠΤΥΧΙΑΚΩΝ ΣΠΟΥΔΩΝ ΠΑΡΑΜΕΤΡΟΙ ΕΠΗΡΕΑΣΜΟΥ ΤΗΣ ΑΝΑΓΝΩΣΗΣ- ΑΠΟΚΩΔΙΚΟΠΟΙΗΣΗΣ ΤΗΣ BRAILLE
ΑΓΓΛΙΚΑ Ι. Ενότητα 7α: Impact of the Internet on Economic Education. Ζωή Κανταρίδου Τμήμα Εφαρμοσμένης Πληροφορικής
 Ενότητα 7α: Impact of the Internet on Economic Education Τμήμα Εφαρμοσμένης Πληροφορικής Άδειες Χρήσης Το παρόν εκπαιδευτικό υλικό υπόκειται σε άδειες χρήσης Creative Commons. Για εκπαιδευτικό υλικό, όπως
Ενότητα 7α: Impact of the Internet on Economic Education Τμήμα Εφαρμοσμένης Πληροφορικής Άδειες Χρήσης Το παρόν εκπαιδευτικό υλικό υπόκειται σε άδειες χρήσης Creative Commons. Για εκπαιδευτικό υλικό, όπως
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ. Πτυχιακή διατριβή Η ΚΑΤΑΘΛΙΨΗ ΩΣ ΠΑΡΑΓΟΝΤΑΣ ΚΙΝΔΥΝΟΥ ΓΙΑ ΑΠΟΠΕΙΡΑ ΑΥΤΟΚΤΟΝΙΑΣ
 ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ Πτυχιακή διατριβή Η ΚΑΤΑΘΛΙΨΗ ΩΣ ΠΑΡΑΓΟΝΤΑΣ ΚΙΝΔΥΝΟΥ ΓΙΑ ΑΠΟΠΕΙΡΑ ΑΥΤΟΚΤΟΝΙΑΣ Παναγιώτου Νεοφύτα 2008969752 Επιβλέπων καθηγητής Δρ. Νίκος Μίτλεττον,
ΤΕΧΝΟΛΟΓΙΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΚΥΠΡΟΥ ΣΧΟΛΗ ΕΠΙΣΤΗΜΩΝ ΥΓΕΙΑΣ Πτυχιακή διατριβή Η ΚΑΤΑΘΛΙΨΗ ΩΣ ΠΑΡΑΓΟΝΤΑΣ ΚΙΝΔΥΝΟΥ ΓΙΑ ΑΠΟΠΕΙΡΑ ΑΥΤΟΚΤΟΝΙΑΣ Παναγιώτου Νεοφύτα 2008969752 Επιβλέπων καθηγητής Δρ. Νίκος Μίτλεττον,
Επιβλέπουσα Καθηγήτρια: ΣΟΦΙΑ ΑΡΑΒΟΥ ΠΑΠΑΔΑΤΟΥ
 EΛΛΗΝΙΚΗ ΔΗΜΟΚΡΑΤΙΑ ΕΚΠΑΙΔΕΥΤΙΚΟ ΤΕΧΝΟΛΟΓΙΚΟ ΙΔΡΥΜΑ ΤΕΙ ΙΟΝΙΩΝ ΝΗΣΩΝ ΤΜΗΜΑ ΔΗΜΟΣΙΩΝ ΣΧΕΣΕΩΝ & ΕΠΙΚΟΙΝΩΝΙΑΣ Ταχ. Δ/νση : Λεωφ. Αντ.Τρίτση, Αργοστόλι Κεφαλληνίας Τ.Κ. 28 100 τηλ. : 26710-27311 fax : 26710-27312
EΛΛΗΝΙΚΗ ΔΗΜΟΚΡΑΤΙΑ ΕΚΠΑΙΔΕΥΤΙΚΟ ΤΕΧΝΟΛΟΓΙΚΟ ΙΔΡΥΜΑ ΤΕΙ ΙΟΝΙΩΝ ΝΗΣΩΝ ΤΜΗΜΑ ΔΗΜΟΣΙΩΝ ΣΧΕΣΕΩΝ & ΕΠΙΚΟΙΝΩΝΙΑΣ Ταχ. Δ/νση : Λεωφ. Αντ.Τρίτση, Αργοστόλι Κεφαλληνίας Τ.Κ. 28 100 τηλ. : 26710-27311 fax : 26710-27312
Repeated measures Επαναληπτικές μετρήσεις
 ΠΡΟΒΛΗΜΑ Στο αρχείο δεδομένων diavitis.sav καταγράφεται η ποσότητα γλυκόζης στο αίμα 10 ασθενών στην αρχή της χορήγησης μιας θεραπείας, μετά από ένα μήνα και μετά από δύο μήνες. Μελετήστε την επίδραση
ΠΡΟΒΛΗΜΑ Στο αρχείο δεδομένων diavitis.sav καταγράφεται η ποσότητα γλυκόζης στο αίμα 10 ασθενών στην αρχή της χορήγησης μιας θεραπείας, μετά από ένα μήνα και μετά από δύο μήνες. Μελετήστε την επίδραση
Αναερόβια Φυσική Κατάσταση
 Αναερόβια Φυσική Κατάσταση Γιάννης Κουτεντάκης, BSc, MA. PhD Αναπληρωτής Καθηγητής ΤΕΦΑΑ, Πανεπιστήµιο Θεσσαλίας Περιεχόµενο Μαθήµατος Ορισµός της αναερόβιας φυσικής κατάστασης Σχέσης µε µηχανισµούς παραγωγής
Αναερόβια Φυσική Κατάσταση Γιάννης Κουτεντάκης, BSc, MA. PhD Αναπληρωτής Καθηγητής ΤΕΦΑΑ, Πανεπιστήµιο Θεσσαλίας Περιεχόµενο Μαθήµατος Ορισµός της αναερόβιας φυσικής κατάστασης Σχέσης µε µηχανισµούς παραγωγής
ΙΠΛΩΜΑΤΙΚΗ ΕΡΓΑΣΙΑ. ΘΕΜΑ: «ιερεύνηση της σχέσης µεταξύ φωνηµικής επίγνωσης και ορθογραφικής δεξιότητας σε παιδιά προσχολικής ηλικίας»
 ΠΑΝΕΠΙΣΤΗΜΙΟ ΑΙΓΑΙΟΥ ΣΧΟΛΗ ΑΝΘΡΩΠΙΣΤΙΚΩΝ ΕΠΙΣΤΗΜΩΝ ΤΜΗΜΑ ΕΠΙΣΤΗΜΩΝ ΤΗΣ ΠΡΟΣΧΟΛΙΚΗΣ ΑΓΩΓΗΣ ΚΑΙ ΤΟΥ ΕΚΠΑΙ ΕΥΤΙΚΟΥ ΣΧΕ ΙΑΣΜΟΥ «ΠΑΙ ΙΚΟ ΒΙΒΛΙΟ ΚΑΙ ΠΑΙ ΑΓΩΓΙΚΟ ΥΛΙΚΟ» ΙΠΛΩΜΑΤΙΚΗ ΕΡΓΑΣΙΑ που εκπονήθηκε για τη
ΠΑΝΕΠΙΣΤΗΜΙΟ ΑΙΓΑΙΟΥ ΣΧΟΛΗ ΑΝΘΡΩΠΙΣΤΙΚΩΝ ΕΠΙΣΤΗΜΩΝ ΤΜΗΜΑ ΕΠΙΣΤΗΜΩΝ ΤΗΣ ΠΡΟΣΧΟΛΙΚΗΣ ΑΓΩΓΗΣ ΚΑΙ ΤΟΥ ΕΚΠΑΙ ΕΥΤΙΚΟΥ ΣΧΕ ΙΑΣΜΟΥ «ΠΑΙ ΙΚΟ ΒΙΒΛΙΟ ΚΑΙ ΠΑΙ ΑΓΩΓΙΚΟ ΥΛΙΚΟ» ΙΠΛΩΜΑΤΙΚΗ ΕΡΓΑΣΙΑ που εκπονήθηκε για τη
Η ΨΥΧΙΑΤΡΙΚΗ - ΨΥΧΟΛΟΓΙΚΗ ΠΡΑΓΜΑΤΟΓΝΩΜΟΣΥΝΗ ΣΤΗΝ ΠΟΙΝΙΚΗ ΔΙΚΗ
 ΑΡΙΣΤΟΤΕΛΕΙΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΘΕΣΣΑΛΟΝΙΚΗΣ ΝΟΜΙΚΗ ΣΧΟΛΗ ΠΡΟΓΡΑΜΜΑ ΜΕΤΑΠΤΥΧΙΑΚΩΝ ΣΠΟΥΔΩΝ ΤΟΜΕΑΣ ΙΣΤΟΡΙΑΣ ΦΙΛΟΣΟΦΙΑΣ ΚΑΙ ΚΟΙΝΩΝΙΟΛΟΓΙΑΣ ΤΟΥ ΔΙΚΑΙΟΥ Διπλωματική εργασία στο μάθημα «ΚΟΙΝΩΝΙΟΛΟΓΙΑ ΤΟΥ ΔΙΚΑΙΟΥ»
ΑΡΙΣΤΟΤΕΛΕΙΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΘΕΣΣΑΛΟΝΙΚΗΣ ΝΟΜΙΚΗ ΣΧΟΛΗ ΠΡΟΓΡΑΜΜΑ ΜΕΤΑΠΤΥΧΙΑΚΩΝ ΣΠΟΥΔΩΝ ΤΟΜΕΑΣ ΙΣΤΟΡΙΑΣ ΦΙΛΟΣΟΦΙΑΣ ΚΑΙ ΚΟΙΝΩΝΙΟΛΟΓΙΑΣ ΤΟΥ ΔΙΚΑΙΟΥ Διπλωματική εργασία στο μάθημα «ΚΟΙΝΩΝΙΟΛΟΓΙΑ ΤΟΥ ΔΙΚΑΙΟΥ»
